Notes
THE FIVE TYPES OF HEPATITIS
Hepatitis is a viral infection which causes liver inflammation. Hepatitis comes from the Ancient Greek word “hepat” which means liver and the Latin word “itis” which means inflammation.
There are five types of hepatitis, which is named after the virus that causes it. The five types are Hepatitis A (HAV), Hepatitis B (HBV), Hepatitis C (HCV), Hepatitis D (HDV), and Hepatitis E (HEV). Among these types, Hepatitis A and E are caused by the ingestion of contaminated food or water. Hepatitis B, C, and D are usually transmitted by contaminated blood or blood products, invasive medical procedures that used contaminated equipment, transmission from mother to baby at birth, from family member to child, and by sexual contact.
TYPES OF HEPATITIS
Hepatitis A
Hepatitis A virus is usually present in the faeces of infected persons and is transmitted by consumption of contaminated food or water. Anal-oral contact during sex can also be a cause of hepatitis A. Since this infection is mild in many cases, most people make a full recovery and do not lead to chronic disease. However, it can also be severe and life-threatening since most areas in the world have poor sanitation.
Hepatitis B
It is a sexually transmitted disease which is caused by the virus HBV. It is usually spread by contact with infected blood, semen, and some other body fluids. One can also be infected by:
- Being bitten by an infected person.
- Transfusions of HBV-contaminated blood and blood products.
- Use of contaminated injections during medical procedures.
- Sharing personal items such as razors with an infected person.
- Using a mother’s milk that is infected to feed a baby.
Hepatitis C
HCV is spread by direct contact with the blood of an infected person. But unlike in persons with Hepatitis B, liver cancer is only increased in people with cirrhosis and only a few Hepatitis C patients get cirrhosis. This is because their liver swells and becomes damaged.
Hepatitis D
Occurs only to patients who are infected with HBV. The combination of HBV and HDV infection result in a more serious disease with a worse outcome. Though the Hepatitis B vaccine can provide protection for Hepatitis D, the infection can still come through contact with infected blood, unprotected sex, and perforation of the skin with infected needles.
Hepatitis E
Like Hepatitis A, Hepatitis E is transmitted through the consumption of contaminated water or food. The spread of HEV is common in developing countries, which is why it is seen as an important cause of hepatitis outbreaks. Though an infected person’s liver swells, there is no long-term consequence for it.
Common Symptoms of Hepatitis
People with hepatitis are undiagnosed because they’ve mistaken it for flu and sometimes there are no symptoms at all. The most common symptoms of hepatitis include:
- Loss of appetite
- Fatigue
- Mild fever
- Muscle or joint aches
- Nausea and vomiting
- Abdominal pain
- Diarrhea
- Vomiting
- Weight loss
Sometimes, there are other symptoms like:
- Dark urine
- Internal bleeding
- Generalized itching.
- Jaundice
- Light-colored stools
Prevention of Hepatitis
Many actions can be taken to reduce the chance of being infected by hepatitis. Though there are safe and effective vaccines available to prevent HAV and HBV, the vaccine for HEV is not widely available. Up to this date, there is still no vaccine for HCV.
- Get vaccines for hepatitis A and B.
- Wash your hands with soap after going to the toilet.
- Consume only cooked foods.
- Avoid tap water when traveling to certain countries or regions.
- Don’t share drug needles, inhalant devices, or take drugs.
- Use a latex condom and practice safe sex.
- Don’t use an infected person’s personal items such as razors or toothbrushes.
- Take precautions when getting tattoos, body piercing, or manicures and pedicures. If possible, bring your own manicure kit. Make sure that the instruments are cleaned or disposable.
- Take precautions too when traveling to areas with poor sanitation.
Discover more from Nursing In Ghana
Subscribe to get the latest posts sent to your email.
Notes
Understanding Hypotension: Types, Causes, and Symptoms
Hypotension, commonly referred to as “low blood pressure,” is a medical condition in which the blood pressure in the arteries is lower than normal (when the blood pressure reading is lower than 90/60mmHg). There are various types of hypotension, each with different causes, symptoms, and treatments. As a nurse, it is important to be aware of the different types of hypotension and their management in order to provide safe and effective care to your patients.
Orthostatic hypotension
Orthostatic hypotension is a type of hypotension that occurs when a person changes position from lying down or sitting to standing up. This can cause a sudden drop in blood pressure, leading to symptoms such as dizziness, lightheadedness, and fainting. Orthostatic hypotension is common in older adults, especially those with underlying medical conditions such as Parkinson’s disease, diabetes, or autonomic neuropathy.
The management of orthostatic hypotension involves lifestyle modifications, such as avoiding sudden changes in position, staying hydrated, and wearing compression stockings. Medications such as fludrocortisone, midodrine, and droxidopa may also be prescribed to help raise blood pressure.
Neurally mediated hypotension.
Neurally mediated hypotension also known as the fainting reflex, neurocardiogenic syncope, vasodepressor syncope, the vaso-vagal reflex, and autonomic dysfunction is a type of hypotension that occurs in response to certain triggers, such as standing for a long time or exposure to heat. It is caused by a malfunction of the autonomic nervous system, which regulates blood pressure and heart rate. Neurally mediated hypotension can cause symptoms such as dizziness, nausea, and fainting. Other symptoms may include confusion, muscle aches, headaches, and chronic fatigue.
The treatment of neurally mediated hypotension involves avoiding triggers and increasing fluid and salt intake.
Severe hypotension
Severe hypotension is a medical emergency that requires immediate treatment. It is characterized by a sudden and severe drop in blood pressure, which can lead to organ damage and even death if not promptly addressed. Severe hypotension can be caused by various conditions, such as sepsis, anaphylaxis, or a heart attack.
The management of severe hypotension involves identifying and treating the underlying cause. This may involve administering intravenous fluids, medications such as vasopressors or inotropes, and oxygen therapy. In severe cases, mechanical ventilation or extracorporeal membrane oxygenation (ECMO) may be necessary.
Postprandial hypotension
It is common in older adults and those with underlying medical conditions such as diabetes, Parkinson’s disease, or autonomic neuropathy. Postprandial hypotension is a type of hypotension that occurs after eating a meal. After eating, the heart rate ramps up to send blood flowing to the digestive system, but with this type of low blood pressure, the mechanism fails, resulting in dizziness, lightheadedness, and fainting.
The management of postprandial hypotension involves eating smaller, more frequent meals and avoiding large meals high in carbohydrates or fats. Medications such as acarbose, midodrine, and caffeine may also be prescribed.
Discover more from Nursing In Ghana
Subscribe to get the latest posts sent to your email.
Notes
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE), A COMMONLY MISDIAGNOSED MEDICAL CONDITION
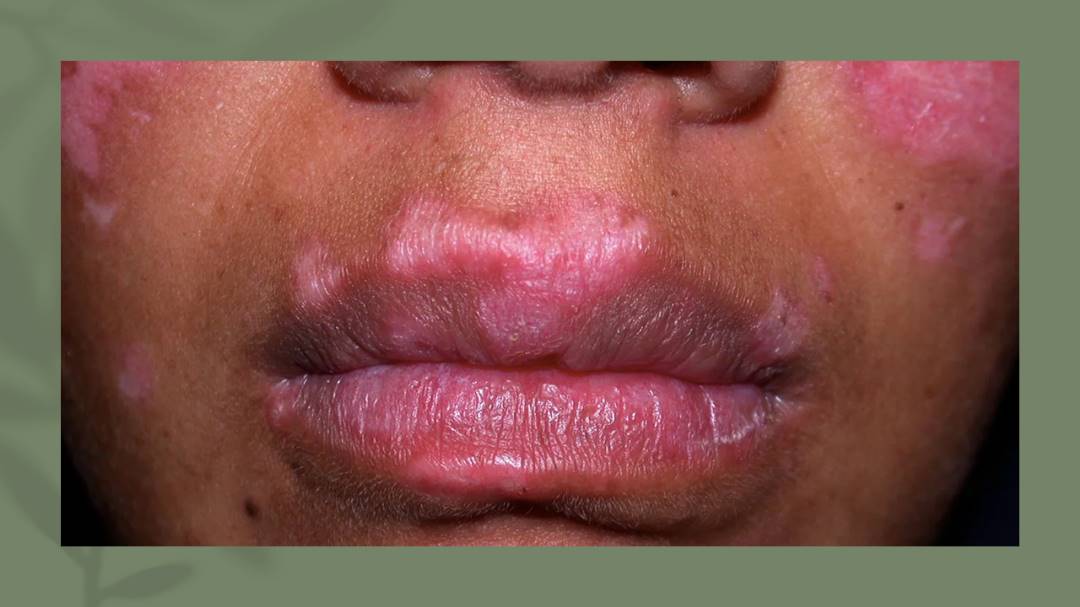
Systemic Lupus Erythematosus (SLE) is a chronic autoimmune disease that can affect various organ systems in the body. It is characterized by the production of autoantibodies against self-antigens, leading to chronic inflammation and tissue damage including the joints, skin, kidneys, blood cells, brain, heart, and lungs. SLE is a heterogeneous disease with a wide range of clinical manifestations, making it difficult to diagnose and manage.
PATHOPHYSIOLOGY
The pathophysiology of SLE involves a complex interplay between genetic, environmental, hormonal, and immunologic factors. Multiple genetic loci have been associated with SLE, including genes involved in immune system function and regulation. Environmental factors such as infections, medications, and ultraviolet light exposure have also been implicated in the development of SLE.
In SLE, immune dysregulation leads to the production of autoantibodies against nuclear components such as DNA, RNA, and histones. These autoantibodies form immune complexes that deposit in various tissues, leading to chronic inflammation and tissue damage. Additionally, immune dysregulation can lead to aberrant T-cell activation, cytokine production, and complement activation, further contributing to the pathogenesis of SLE.
CAUSES
The exact causes of SLE are not fully understood, but a combination of genetic, environmental, hormonal, and immunologic factors are thought to contribute to its development. Women are more commonly affected than men, and the disease often presents during the childbearing years. Genetic factors are estimated to account for up to 66% of the risk for developing SLE. Environmental factors such as infections, medications, and ultraviolet light exposure have also been implicated in the development of SLE.
CLINICAL MANIFESTATIONS
The clinical manifestations of SLE are diverse and can affect multiple organ systems in the body. Common symptoms include fatigue, fever, joint pain and swelling, skin rashes, and photosensitivity. SLE can also cause more serious complications such as lupus nephritis, which is a major cause of morbidity and mortality in patients with SLE.
ASSESSMENT AND DIAGNOSTIC FINDINGS
The diagnosis of SLE is based on a combination of clinical and laboratory findings. The American College of Rheumatology has developed diagnostic criteria for SLE, which require the presence of at least four of the following: malar rash, discoid rash, photosensitivity, oral ulcers, arthritis, serositis, renal disorder, neurologic disorder, hematologic disorder, immunologic disorder, and antinuclear antibody positivity. Laboratory tests that may be helpful in diagnosing SLE include antinuclear antibody (ANA) testing, anti-double-stranded DNA (anti-dsDNA) antibody testing, and complement-level testing.
MEDICAL MANAGEMENT
The management of SLE involves a multidisciplinary approach, including rheumatologists, nephrologists, dermatologists, and other specialists as needed. Treatment goals include controlling disease activity, preventing flares, and minimizing organ damage. Treatment options may include nonsteroidal anti-inflammatory drugs (NSAIDs), antimalarial drugs, glucocorticoids, immunosuppressants, and biological agents.
PHARMACOLOGIC MANAGEMENT
Pharmacologic management of SLE involves a range of medications targeting different aspects of the disease’s pathophysiology. NSAIDs can be used to manage mild to moderate pain and inflammation, while antimalarial drugs such as hydroxychloroquine can be used to prevent disease flares and reduce disease activity. Glucocorticoids such as prednisone can be used to manage severe disease activity and organ involvement, but their long-term use is associated with significant adverse effects. Immunosuppressive agents such as azathioprine, mycophenolate mofetil, and cyclophosphamide can be used to control disease activity and prevent organ damage. Biologic agents such as belimumab, a monoclonal antibody targeting B-cell activating factor, have also been approved for the treatment of SLE.
Systemic lupus erythematosus diagnosis and management, https://academic.oup.com/rheumatology/article/56/suppl_1/i3/2738661.
C. (2023, January 31). Systemic lupuserythematosus (SLE). Centers for Disease Control and Prevention. https://www.cdc.gov/lupus/facts/detailed.html
Systemic lupus erythematosus pathophysiology – wikidoc. (n.d.). Systemic Lupus Erythematosus Pathophysiology – Wikidoc. https://www.wikidoc.org/index.php/Systemic_lupus_erythematosus_pathophysiology
Discover more from Nursing In Ghana
Subscribe to get the latest posts sent to your email.
Notes
TYPES OF SHOCK
Shock is a threatening life condition of circulatory failure which causes inadequate oxygen delivery to meet cellular metabolic needs and oxygen consumption requirements, producing cellular and tissue hypoxia. The effects of shock are initially reversible, but rapidly become irreversible, resulting in multiorgan failure (MOF) and death. When a patient presents with undifferentiated shock, it is important that the clinician immediately initiate therapy while rapidly identifying the etiology so that definitive therapy can be administered to reverse shock and prevent MOF and death.
There are four main types of shock:
1. Anaphylactic shock
2. Cardiogenic shock
3. Hypovolemic shock
4. Septic shock
Anaphylactic shock is a severe and sudden allergic reaction that can occur after exposure to an allergen. Symptoms include swelling of the face and throat, difficulty breathing, and a drop in blood pressure. Anaphylactic shock can be life-threatening and requires immediate medical treatment.
Cardiogenic shock occurs when the heart is unable to pump enough blood to meet the body’s needs. This can be due to a heart attack, heart failure, or other heart conditions. Symptoms include shortness of breath, chest pain, and a weak and irregular heartbeat. Cardiogenic shock is a medical emergency and requires treatment in a hospital.
Hypovolemic shock occurs when there is a decrease in the amount of blood or fluid in the body. This can be due to blood loss from an injury, severe dehydration, or excessive vomiting or diarrhea. Symptoms include lightheadedness, fainting, and a decrease in urine output. Hypovolemic shock can be life-threatening and requires immediate medical treatment.
Septic shock. This type of shock is caused by an infection or sepsis. Sepsis is a potentially life-threatening condition that occurs when an infection spreads throughout the body. Symptoms include low blood pressure, rapid heart rate, chills, and fever. Septic shock is a medical emergency and requires treatment in a hospital.
Discover more from Nursing In Ghana
Subscribe to get the latest posts sent to your email.
-

 Nursing News5 years ago
Nursing News5 years agoLIST OF ACCREDITED GOVERNMENT NURSING AND MIDWIFERY TRAINING SCHOOLS IN GHANA
-

 Nursing News3 years ago
Nursing News3 years agoNURSING ADMISSION FORMS ON SALE FOR THE 2023/2024 ACADEMIC YEAR
-

 Nursing Procedures and Skills5 years ago
Nursing Procedures and Skills5 years agoTHE NURSES PLEDGE AND THE MIDWIVE’S PRAYER
-

 Nursing Procedures and Skills5 years ago
Nursing Procedures and Skills5 years agoNURSING TRAINING ADMISSION INTERVIEW QUESTIONS
-

 Nursing News4 years ago
Nursing News4 years agoGHS INTRODUCES TWO NEW BELT COLOURS FOR TWO NEW LEVELS IN THE NURSING AND MIDWIFERY SERVICE
-

 Nursing News5 years ago
Nursing News5 years agoMOH SUSPENDS THE 2021/2022 ACADEMIC CALENDAR FOR NURSING AND MIDWIFERY SCHOOLS
-
 Notes5 years ago
Notes5 years agoCOMMON TYPES OF INTRAVENOUS (IV) FLUIDS AND THEIR USES
-

 Nursing News5 years ago
Nursing News5 years agoLIST OF PRIVATE NURSING AND MIDWIFERY TRAINING SCHOOLS (ACCREDITED)